Modern dentistry offers many reliable ways to replace missing teeth, and removable dentures remain a practical, time-tested option for restoring a healthy, confident smile. While dental implants and fixed bridgework are excellent solutions for many patients, dentures continue to provide a versatile approach that suits a wide range of oral health needs.
At Smiles N Beyond in Wallington, NJ, we fabricate dentures using durable, lifelike materials and thoughtful design so they feel comfortable and look natural. Our team prioritizes an individualized approach — matching each prosthesis to the patient's facial proportions, speech needs, and daily routines.
This page explains how tooth loss affects your mouth and overall wellbeing, what modern dentures are, the different types available, how we design them for lasting function, and what to expect as you adapt to a new prosthesis. The goal is to give you clear, useful information so you can make informed choices about tooth replacement.
Losing one or more teeth does more than leave a visible gap. Missing teeth alter the way your bite works, change how forces are distributed across the jaw, and can make chewing less efficient. Over time, these changes can affect the alignment of remaining teeth and lead to wear or shifting that creates new dental problems.
There are also effects on facial support: teeth and roots help preserve the contours of the jaw and lower face. When teeth are absent, the underlying bone gradually remodels and can shrink, which subtly changes facial proportions and can make the lower face appear less full. Dentures restore visible tooth structure and help support facial tissues to maintain a more balanced profile.
Beyond the physical impact, tooth loss can influence social confidence and everyday comfort. Difficulty pronouncing certain sounds, reduced enjoyment of favorite foods, or self-consciousness about smiling are common concerns. Replacing missing teeth with a well-made denture can address these issues and improve quality of life for many people.
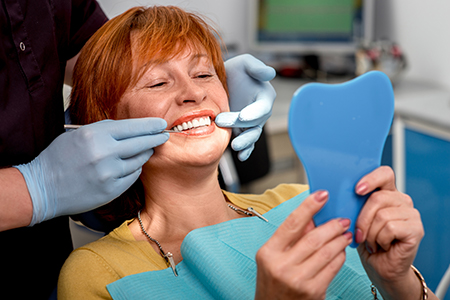
Dentures are removable prosthetic devices that replace missing teeth and the surrounding gum tissue. They sit over the gums and distribute biting forces across the soft tissues and residual ridge. The visible portion consists of artificial teeth set into a supportive base that is shaped and colored to match natural gums.
Because dentures are removable, they offer some practical benefits: they can be taken out for cleaning, allow full inspection of the tissues underneath, and make daily oral hygiene more straightforward in many cases. At the same time, modern denture materials and fabrication methods allow for highly esthetic results that mimic natural teeth and smile lines.
Depending on the clinical situation, dentures can be designed for stability, comfort, and function — from lightweight partials that replace a few teeth to complete prostheses that restore an entire arch. The right solution depends on the number of teeth missing, the health of the remaining teeth and gums, and the patient's personal preferences.
A careful clinical evaluation is essential to determine whether a partial or complete denture is the best path forward. We examine the condition of remaining teeth, the shape and volume of supporting bone, soft tissue health, and how the jaws come together. All of these factors influence design choices and expected long-term performance.
Removable dentures fall broadly into two categories: full (complete) dentures, which replace all teeth in an arch, and partial dentures, which fill gaps when some natural teeth remain. New materials and attachment options have also expanded the ways dentures can be stabilized and supported for improved function.
Every denture is custom-made, and the process includes careful records, impressions, and trial fittings to balance function, comfort, and esthetics. Patient input is important throughout; selecting tooth shape, shade, and the overall appearance helps ensure results that feel and look right for each individual.
Complete dentures replace all teeth in the upper arch, lower arch, or both. They are an appropriate choice when remaining teeth cannot be maintained or when extraction of the remaining dentition is recommended. A well-made full denture restores chewing surfaces, supports the lips and cheeks, and recreates a natural smile line.
An immediate denture can be placed at the time teeth are removed so patients do not go without teeth during healing. Because the tissues change as they heal, immediate prostheses often require follow-up adjustments or relines to maintain fit.
Conventional full denture
A conventional full denture is made after the gums and bone have healed following extractions. Fabricating the prosthesis on a healed ridge helps achieve a precise fit and stable function.
Overdenture
An overdenture gains extra retention from existing tooth roots or specially placed attachments, preserving bone and improving stability compared with a traditional complete denture.
Implant-supported dentures
Implant-supported options anchor the denture to small titanium posts placed in the jaw, offering enhanced retention and reduced movement — particularly helpful for lower-arch prostheses where stability can be more challenging.
Partial dentures are designed to fill spaces left by one or more missing teeth while preserving healthy natural teeth. They commonly attach to adjacent teeth with clasps or precision attachments and can prevent drifting of neighboring teeth, helping maintain proper bite relationships.
Modern partial frameworks are made from a variety of materials, including cast metal for strength, flexible acrylics for comfort, or hybrid materials that balance durability and aesthetics. The design is tailored to minimize bulk while providing reliable support for chewing and speaking.
Whether a partial denture is a temporary or long-term solution depends on each patient's needs. Proper planning and careful fabrication help ensure that a partial integrates smoothly with remaining dental work and daily function.
Throughout the planning and fabrication process, our focus is on delivering a denture that looks natural, fits comfortably, and restores function so you can speak, smile, and eat with confidence.

Creating a successful denture involves both technical accuracy and an eye for aesthetics. We begin with a thorough oral exam and diagnostic imaging as needed, then take precise impressions and jaw relationship records. These steps allow us to plan tooth position, bite, and the contour of the prosthetic base for optimal comfort and function.
Technical details matter: occlusion (how the teeth meet), the vertical dimension of the bite, and the way the prosthesis interacts with lips and cheeks all affect speech, chewing efficiency, and long-term comfort. Our laboratory partners and clinical team work together through try-ins and adjustments until the prosthesis meets these functional and esthetic goals.
For many patients, additional procedures prior to denture fabrication — such as minor soft-tissue contouring or the careful preparation of remaining teeth — will improve fit and longevity. Where appropriate, implant-retained attachments can be incorporated to increase stability and reduce movement during chewing.
We also emphasize patient education: learning how to insert and remove the denture, how to clean it properly, and how to care for the tissues beneath it all contribute to a successful long-term outcome.

Adjusting to a new denture takes time, patience, and a few practical strategies. Speech and chewing may feel different at first; most patients find that reading aloud and starting with soft, manageable foods helps retrain the muscles of the mouth. Short, frequent practice sessions with speaking and eating accelerate adaptation.
Managing fit and sore spots
Small areas of irritation are common early on. If you notice a sore spot, wearing the denture until your adjustment appointment can help the clinician identify and relieve the exact area causing pressure.
Temporary increase in saliva
The presence of a new appliance can stimulate saliva production at first. This reaction typically subsides as your mouth becomes accustomed to the prosthesis.
Speaking and eating with confidence
Practice is the key: start by chewing on both sides, cut food into smaller pieces, and avoid sticky items until you feel secure. Speaking exercises and repetition will usually restore normal clarity within days to a few weeks.
Cleaning and daily care
Rinse dentures after meals and brush them daily with a soft brush designed for prostheses to remove food and biofilm. Soak them overnight in water or a recommended cleaner to keep them free of stains and odor.
Continue to clean any remaining natural teeth and the gums beneath the denture. Healthy tissues improve comfort and help preserve the shape of the supporting ridge.
Remove your dentures at night to give tissues a rest and to reduce the risk of irritation or infection.
Improving stability
Denture adhesives can help in some cases, but implant attachments or precision connectors offer a more predictable improvement in retention for patients who need it.
Routine checkups and relines
Regular follow-up visits let us monitor fit, oral tissue health, and the condition of your denture. Over time tissues change and a reline or adjustment may be recommended to restore a secure, comfortable fit.
If you have questions about which denture option is right for you or want to learn more about the steps involved, our team is ready to help. Contact us to discuss your needs and schedule a consultation — we’ll provide a thoughtful assessment and guide you toward a solution that supports your health and daily life.

Dentures are removable prosthetic devices that replace missing teeth and the surrounding gum tissue, restoring the visible structure of the dental arch. They sit over the gums and transfer biting forces to the soft tissues and residual ridge, helping you chew and speak more effectively. Modern denture materials and fabrication techniques allow for lifelike tooth shapes and gum tones that mimic natural dentition.
The base of a denture is contoured to match the mouth and provide support for the artificial teeth, while retention comes from fit, muscle control, and, when used, attachments or implants. Because they are removable, dentures can be taken out for cleaning and inspection of the tissues underneath, which supports ongoing oral hygiene. Proper design balances esthetics, function, and comfort to help restore normal daily activities such as eating and speaking.
Complete dentures replace all teeth in an upper or lower arch and are used when the remaining teeth cannot be preserved or when full extraction is planned. Partial dentures fill gaps when some natural teeth remain and typically attach to adjacent teeth using clasps or precision attachments to maintain space and prevent drifting. The choice between complete and partial depends on the number of missing teeth, the health of the remaining teeth and gums, and the desired long-term plan for oral health.
Partial frameworks can be made from metal, flexible acrylic, or hybrid materials to balance strength and comfort, while complete dentures are designed to support facial tissues and recreate a natural smile line. Each prosthesis is custom-made through impressions, bite records, and try-ins to ensure proper function with the existing dentition. Patient goals and clinical findings guide the final design and material selection.
An immediate denture is placed at the time teeth are removed so the patient does not remain without teeth during healing; it often requires follow-up relines or adjustments because the tissues change during recovery. A conventional denture is fabricated after the gums and bone have healed following extractions and typically provides a more precise fit on a stable ridge. Implant-supported dentures use dental implants to anchor the prosthesis, offering improved retention and reduced movement compared with traditional removable options.
Overdentures are a hybrid approach that preserve roots or use attachments to enhance stability and help preserve bone. Implant-retained options are particularly helpful for lower-arch prostheses where stability is more challenging due to ridge shape and muscle activity. Your clinician will explain the advantages and limitations of each approach based on your oral anatomy and functional needs.
Good candidates for dentures include patients with multiple missing teeth, those whose remaining teeth are not salvageable, and individuals seeking a removable tooth-replacement option that restores appearance and basic function. The clinical evaluation will examine gum health, bone volume, the condition of remaining teeth, and bite relationships to determine whether a partial or complete denture is appropriate. Medical history and oral conditions such as dry mouth or oral lesions are also considered because they can influence denture fit and tissue health.
When appropriate, planning may incorporate implant retention or overdenture design to improve comfort and stability for patients with low ridge height or high functional demands. A thorough consultation and diagnostic workup, including imaging when needed, help identify the safest and most effective denture solution for each individual. Shared decision-making between the patient and clinician ensures the chosen option aligns with functional goals and daily lifestyle.
Successful denture fabrication begins with a comprehensive oral exam and diagnostic records, including impressions and jaw relationship measurements to establish proper tooth position and vertical dimension. These records guide the laboratory in creating trial prostheses so that bite, esthetics, and phonetics can be evaluated and adjusted before the final prosthesis is processed. Attention to occlusion, the way the teeth meet, and the contour of the base that interacts with lips and cheeks is critical to long-term comfort and function.
Fabrication typically involves multiple appointments for try-ins and refinements to ensure the denture meets functional and esthetic goals. Minor soft-tissue procedures or selective preparation of remaining teeth may be recommended beforehand to improve fit and longevity. Collaboration between the clinical team and dental laboratory allows for precise control of tooth shade, shape, and position to achieve a natural appearance that supports speech and chewing.
Adaptation to new dentures varies, but many patients notice progressive improvements in comfort, speech, and chewing over days to a few weeks as oral muscles learn to control the prosthesis. Reading aloud, speaking slowly, and practicing with soft, easy-to-chew foods accelerate the retraining of speech and chewing patterns. Short, frequent sessions of eating and speaking help build confidence and reduce the risk of sore spots from uneven pressure.
Minor soreness and increased saliva production are common initially and usually resolve as the tissues adapt, but persistent irritation should be evaluated so the denture can be adjusted. Wearing the denture to follow-up appointments allows the clinician to precisely locate and relieve areas of pressure. Patience, practice, and regular communication with your dental team are the most effective strategies for a smooth transition.
Daily care begins with rinsing dentures after meals to remove loose food and brushing them daily with a soft brush designed for prostheses to remove biofilm and stains. Dentures should be soaked overnight in water or a recommended denture cleaner to maintain hygiene and prevent odor, while any remaining natural teeth and the gums beneath the denture must also be cleaned to support tissue health. Removing dentures at night gives the oral tissues a rest and reduces the risk of irritation or infection.
Regular inspection of the prosthesis for cracks, wear, or changes in fit helps catch issues early and prevents further complications. Avoid abrasive cleaners and hot water, which can damage denture materials or alter fit. Routine dental visits allow your clinician to monitor tissue health, perform professional cleaning when needed, and recommend relines or repairs as tissues change over time.
Non-surgical approaches to improve denture stability include relines to restore intimate contact with the supporting tissues, adjustments to occlusion to reduce tipping, and the use of well-fitted precision attachments in partial frameworks. Denture adhesives can provide short-term improvement in retention for some patients, but their effectiveness varies and they are not a substitute for proper fit. Choosing a lightweight, well-contoured denture base and optimizing tooth arrangement can also enhance muscle control and reduce displacement during function.
Regular maintenance and timely relines are important when tissue volume changes lead to looseness, and careful occlusal adjustments can minimize rocking and sore spots. For patients seeking greater retention without full implant surgery, solutions such as conservative root-retained overdentures or strategic attachments to remaining teeth can be explored. Your dentist will review the risks and benefits of each option based on your anatomy and functional expectations.
Dentures should be evaluated routinely because the underlying bone and soft tissues change over time, which can alter fit and function and lead to discomfort or decreased chewing efficiency. Relines are commonly recommended when the denture becomes loose but remains structurally sound, as they restore close adaptation to the ridge without replacing the entire prosthesis. Adjustments to occlusion or pressure-relieving modifications are indicated when sore spots or functional problems arise after delivery.
A denture may need to be remade when wear, fracture, or major anatomical changes prevent achieving adequate fit and esthetics with relines or repairs. Regular follow-up visits let your dental team monitor tissue health, make minor corrections, and determine the appropriate timing for relines or replacement. Prompt attention to changes in fit or comfort helps maintain oral health and preserve the function of the prosthesis.
To schedule a denture consultation, call the office during business hours or use the practice contact form to request an appointment for an initial evaluation and treatment discussion. During the consultation the clinician will review your medical and dental history, perform a thorough oral exam, and discuss the denture options that best match your needs and long-term goals. Diagnostic imaging and impressions may be recommended to create a personalized treatment plan.
Appointments for denture care are typically coordinated to allow adequate time for examination, patient questions, and treatment planning so you understand the steps involved. If you have existing dentures, bring them to the appointment so the team can assess fit and wear patterns. Clear communication about expectations and daily needs helps the dentist recommend the most suitable prosthetic design and follow-up schedule.

Ready to schedule your next dental appointment or have questions about our services?
Getting in touch with Smiles N Beyond is simple. Our friendly team is here to help you schedule appointments, answer questions about treatment options, and address any concerns you may have. Whether you prefer to call our office, send an email, or complete our easy online contact form, we’re happy to assist you. Take the first step toward a healthier, more confident smile, contact us today and experience the difference personalized dental care can make.