
At Smiles N Beyond, our first goal is to preserve your natural teeth whenever it's safe and sensible to do so. Still, extractions remain an essential and sometimes unavoidable part of maintaining oral health. When a tooth threatens adjacent teeth, contributes to infection, or causes ongoing pain, removing it can stop harm and set the stage for a healthier mouth.
We approach every extraction with a focus on clear communication and individualized care. Before recommending removal, our team reviews your dental and medical history, evaluates any imaging, and discusses alternatives so you understand why extraction is being suggested and what the next steps will be.
Understanding the typical reasons a tooth might be taken helps patients feel more informed and less anxious. Below are the common scenarios that lead to an extraction and what each situation generally involves from a treatment perspective.
An over-retained primary (baby) tooth
Sometimes a primary tooth does not loosen and fall out as expected. If the baby tooth’s roots fail to resorb or the tooth fuses to the jawbone, it can block the eruption path of the permanent tooth and disrupt proper alignment. Timely removal of an over-retained primary tooth can prevent crowding and guide healthier development.
Extensive decay that compromises the tooth
Decay begins on the enamel and, if left untreated, can progress deeper into the dentin and pulp. When a tooth has lost too much structure or the infection has severely damaged the root, restoration may no longer be viable. In those cases, extraction eliminates the source of infection and pain and protects neighboring teeth.
Severe fracture or structural failure
Teeth can fracture in many ways. Minor chips may be restored, but when a crack reaches the root or the remaining tooth is insufficient for a durable restoration, removal can be the most predictable option for comfort and oral health.
Advanced periodontal (gum) disease
Periodontal disease erodes the bone and soft tissues that support teeth. In advanced stages, teeth can become loose and painful. Extracting teeth that have been compromised by severe periodontal disease can reduce infection and allow treatment to focus on stabilizing the surrounding teeth and tissues.
Impacted or problematic wisdom teeth
Third molars often lack the space to erupt properly. When wisdom teeth become impacted, decay-prone, or a source of crowding and discomfort, their removal can prevent future complications and protect adjacent teeth.
Overcrowding as part of orthodontic planning
When jaws are too small to accommodate all permanent teeth, selective extractions can be part of an orthodontic plan to create room and help achieve a stable, well-aligned bite. These decisions are made in coordination with an overall treatment plan for the best long-term result.
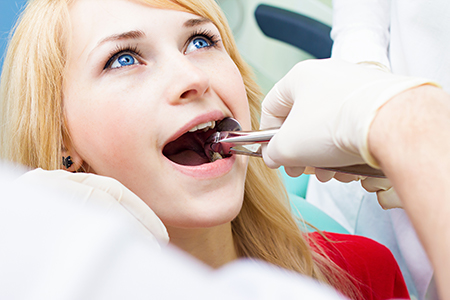
Before any procedure, we complete a thorough review of your health history and any medications you take. That review helps us identify potential risks and determine whether additional precautions — such as pre-procedure antibiotics or medical clearance from your physician — are needed. We’ll explain those steps and answer your questions so you feel prepared.
On the day of the procedure, local anesthesia is used to numb the area and keep you comfortable. For patients with anxiety or complex surgical needs, we also discuss options for dental sedation to help you stay relaxed. Our team monitors comfort and safety throughout the appointment.
To plan the approach, we typically use digital radiographs to assess root shape, bone levels, and the orientation of the tooth. This imaging helps the dentist determine whether a simple extraction will suffice or whether a surgical approach is required. We’ll review the plan with you and outline post-operative expectations before moving forward.
A simple extraction is performed when a tooth is visible in the mouth and the root anatomy is straightforward. After numbing the area, the dentist gently loosens the surrounding ligaments and removes the tooth using forceps. The process is usually quick and predictable, and most patients tolerate it well with only local anesthesia.
Surgical extractions are used for teeth that are broken below the gumline, ankylosed to bone, or impacted. This procedure may involve making a small incision in the gum and, if necessary, removing a bit of bone to access the tooth. In some cases, our office will coordinate care with an oral and maxillofacial surgeon to ensure the best possible outcome for complex situations.
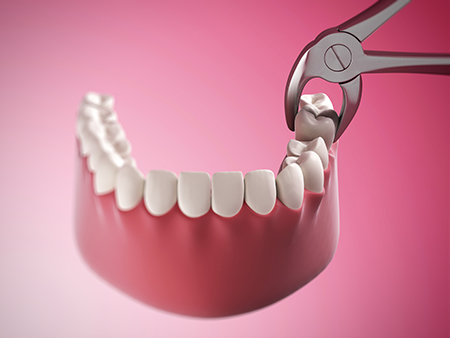
Recovery after extraction varies by the complexity of the procedure and by individual healing. Expect some swelling and mild discomfort that should improve over a few days. Following our post-operative instructions closely is the best way to minimize complications and support a smooth recovery.
Protecting the clot that forms in the socket is essential to healing. Activities that create suction in the mouth — such as using a straw, vigorous rinsing, or smoking — can dislodge the clot and lead to a painful condition called dry socket. We’ll explain specific do’s and don’ts based on your procedure.
We provide guidance about pain control, which may include over-the-counter options or prescribed medications when appropriate. Take any prescribed antibiotics or medications exactly as directed, and contact our team if you have questions about side effects or interactions with other drugs you take.
Maintain gentle pressure
You will be given gauze to bite down on immediately after the extraction to encourage clot formation. Keep firm, steady pressure for the recommended time, and replace the gauze according to the instructions if needed.
Be cautious until numbness wears off
Local anesthetic can blur sensation for a few hours. Avoid chewing or touching the area until normal feeling returns to prevent accidental bites or irritation.
Follow medication directions
If antibiotics are prescribed, complete the full course. For pain, take medications as advised and avoid activities that may increase bleeding or delay healing.
Avoid disturbing the socket
Don’t rinse vigorously, spit forcefully, or use a straw for the first 24–48 hours. These actions can prevent the clot from stabilizing and interfere with healing.
Manage swelling
Applying an ice pack to the outside of the face in 10-minute intervals during the first day can help reduce swelling and discomfort.
Refrain from smoking
Tobacco impairs healing and increases the risk of complications. Avoid smoking for at least one week following extraction.
Stick to gentle foods
Choose soft, lukewarm foods and avoid hot, spicy, or carbonated items while the site is healing. Stay hydrated with non-irritating beverages.
Keep oral hygiene gentle
Continue brushing other teeth carefully and, after the first day, you may rinse gently with a saltwater solution to keep the area clean. Avoid vigorous swishing.
Attend your follow-up appointment
If stitches were placed or follow-up care was recommended, keep your scheduled visit so we can confirm proper healing and address any concerns.
If you notice persistent bleeding, increasing pain, swelling that worsens after a few days, a bad taste in your mouth, or any other unusual symptoms, reach out to our team so we can evaluate and guide next steps.
Once the extraction site has healed, many patients want to know about replacing the missing tooth. Options commonly discussed include dentures, fixed dental bridges, and dental implants. Each choice has distinct benefits and considerations related to durability, maintenance, and how closely it restores natural chewing function.
Dental implants are often recommended when patients seek a solution that closely mimics a natural tooth in function and appearance, while bridges and removable prosthetics remain appropriate in many circumstances depending on the number of missing teeth and the overall treatment plan. We’ll review the advantages and limitations of each approach and tailor recommendations to your goals and clinical needs.
Coordinating restorative planning early—sometimes even before extraction—can preserve bone and simplify future rehabilitation. When appropriate, we’ll explain timing and any preparatory steps so your transition from extraction to replacement is as smooth as possible.
Your safety is central to how we deliver extraction care. Infection-control protocols, careful assessment of medical conditions, and attention to medication interactions all contribute to safer procedures. When a patient’s medical history suggests additional precautions, we collaborate with physicians to obtain the necessary clearances.
We also prioritize your comfort through patient-centered measures: a clear explanation of the procedure, available sedation options for nervous patients, and attentive post-operative guidance. Our goal is to minimize discomfort and uncertainty so you can focus on healing.
When a case benefits from a specialist’s expertise—such as complex surgical extractions or implant placement—we will coordinate referrals and work together to ensure a seamless continuum of care from start to finish.
Tooth extraction is a common, carefully managed treatment that protects oral health when preservation is no longer possible. From initial evaluation and imaging to thoughtful planning for comfort, healing, and eventual replacement, the process is designed to keep you informed and supported at every step. At Smiles N Beyond, we aim to provide compassionate, evidence-based care and clear guidance tailored to each patient's needs.
If you have questions about extractions, recovery, or replacement options, please contact us for more information and to discuss your individual situation.

Tooth extraction becomes necessary when preservation is no longer a safe or predictable option for maintaining oral health. Common reasons include severe decay that destroys tooth structure, advanced periodontal disease that weakens the supporting bone, irreparable fractures, and impacted or problematic wisdom teeth. Extractions are also recommended when a tooth is a persistent source of infection or pain that threatens adjacent teeth or overall health.
Before recommending removal, the dental team reviews your medical and dental history, evaluates images such as digital radiographs, and discusses alternatives when feasible. That assessment helps determine whether root canal treatment, restoration, or other therapies might succeed instead of extraction. Patients are encouraged to ask questions about the rationale and the anticipated next steps so they can make an informed decision.
Appointments begin with a health review and any necessary imaging to evaluate root shape, bone levels, and the tooth's orientation. Local anesthesia is used to numb the area, and for patients who experience anxiety or require complex surgery, sedation options may be discussed to improve comfort and safety. The dentist explains the planned approach and monitors the patient throughout the procedure to ensure steady comfort and a controlled environment.
Simple extractions involve loosening the tooth and removing it with forceps, while surgical extractions may require a small incision, removal of bone, or sectioning the tooth. In cases that are particularly complex, the office coordinates care with an oral and maxillofacial surgeon to provide the appropriate level of expertise. After removal, the team provides specific post-operative instructions to support healing and reduce the risk of complications.
A simple extraction is performed on a tooth that is fully visible in the mouth and has a straightforward root anatomy; it typically requires only local anesthesia and forceps to remove the tooth. The procedure is usually quick and predictable, and most patients experience minimal intervention beyond the extraction itself. Simple extractions are common for primary teeth or permanent teeth that have erupted normally and are free of extensive structural damage.
Surgical extraction is used for teeth that are broken at the gumline, impacted, or fused to the jawbone, and it may involve lifting a small gum flap, removing a bit of bone, or sectioning the tooth into pieces for safer removal. Surgical cases often require additional planning, may use sedation, and can involve a longer recovery period compared with simple extractions. When expertise beyond the general practice is needed, a referral to a specialist helps ensure the best outcome.
Preparation starts with a thorough medical and dental history, including a list of medications, allergies, and underlying health conditions that could affect treatment or healing. If you take blood thinners, are immunocompromised, or have certain cardiac conditions, the dentist may coordinate with your physician to determine the safest approach. For patients planning to use sedation, instructions about fasting and arranging transportation will be provided prior to the appointment.
On the day of the procedure, follow any pre-appointment guidelines your dental team gives regarding medications and eating or drinking. Wear comfortable clothing and bring a list of your current medications and any recent medical updates. Clear communication about anxiety, past reactions to anesthesia, or other concerns helps the team tailor the visit for your comfort and safety.
Recovery time depends on the complexity of the extraction and individual healing responses, but most patients notice steady improvement within a few days to two weeks. Expect some swelling and discomfort that peaks in the first 48 hours and then gradually subsides; using ice packs and following pain management instructions helps reduce discomfort. Normal daily activities can usually resume within a day or two for simple extractions, while surgical cases may require a longer, more cautious recovery period.
Protecting the blood clot that forms in the socket is essential for healing, so avoid actions that create suction in the mouth such as using a straw, vigorous rinsing, or smoking in the immediate post-operative period. Maintain gentle oral hygiene around the site, eat soft foods, and stay hydrated with non-irritating beverages. Keep any scheduled follow-up visits so the dental team can confirm proper healing and address concerns early.
Dry socket occurs when the blood clot that protects the extraction site becomes dislodged, exposing bone and nerves and causing significant pain; avoiding strenuous rinsing, spitting, and using straws in the first 24–72 hours reduces this risk. Tobacco use and excessive physical activity increase the likelihood of dry socket and impaired healing, so patients are strongly advised to refrain from smoking and heavy exertion during the initial healing phase. Following the post-operative instructions for oral hygiene and diet helps protect the clot and promotes uneventful healing.
If your dentist prescribes medications such as antibiotics or specific mouth rinses, take them exactly as directed and report any side effects or concerns. Persistent or worsening pain, unusual drainage, fever, or prolonged bleeding are signs that warrant prompt evaluation. Early communication with the dental team allows timely intervention to address infection, dry socket, or other complications.
Pain after an extraction is typically managed with over-the-counter analgesics such as ibuprofen or acetaminophen used according to the dentist's guidance; these medications reduce inflammation and control discomfort for most patients. In certain situations where greater pain control is required, a short course of prescription medication may be provided, and the dental team will discuss appropriate use and potential side effects. If antibiotics are indicated to manage or prevent infection, they should be taken for the full prescribed course to ensure effectiveness.
Always inform the dentist of other medications you take, including blood thinners and supplements, because interactions can affect bleeding, healing, and medication choices. If you have allergies to specific drugs, that information helps the team select safe alternatives. Use medications only as directed and contact the office with questions about dosing or signs of an adverse reaction.
Contact the dental team promptly if you experience persistent or heavy bleeding beyond the immediate post-operative period, severe pain that does not respond to prescribed pain control, or swelling that worsens after several days. A fever, difficulty breathing or swallowing, a bad taste or odor in the mouth that suggests infection, or numbness that persists longer than expected are also reasons to seek evaluation. These symptoms may indicate infection, dry socket, or another complication that requires timely care.
If you are uncertain whether a symptom is expected or concerning, call so the team can assess your situation and advise next steps. Early intervention often prevents more serious problems and supports a smoother recovery. Keep follow-up appointments and report any new or unusual changes in your condition as they arise.
After healing, common replacement options include removable partial dentures, fixed bridges, and dental implants; each option has distinct benefits related to function, appearance, and long-term oral health. Implants are often recommended for their ability to preserve bone and closely mimic the look and function of a natural tooth, while bridges and removable prosthetics remain appropriate choices depending on the number of missing teeth and the patient's preferences. Your dentist will discuss the pros and cons of each option and tailor recommendations to your clinical needs and goals.
Coordinating restorative planning early, sometimes even before extraction, can help preserve bone and streamline the transition to replacement. When implant placement is planned, the timing—immediate, early, or delayed—depends on factors such as infection, bone volume, and overall health. The team at Smiles N Beyond works with patients to develop a stepwise plan that supports predictable healing and restoration of form and function.
Yes, extractions can play a central role in broader dental treatment plans, including orthodontics and implant-supported restorations, and careful coordination improves outcomes. In orthodontics, selective extractions may create space to align teeth properly and achieve a balanced bite, and those decisions are made in the context of a comprehensive treatment plan. For implant therapy, the condition of the extraction site and the amount of available bone influence whether bone grafting or staged procedures are necessary to support a future implant.
Early communication between specialists and the general dental team allows for planning that preserves bone and optimizes timing for restorative or orthodontic care. Sharing radiographs, medical history, and treatment goals ensures that extractions are performed with an eye toward the next phase of care. Patients should discuss long-term plans with their dentist so each step supports a predictable, functional result.

Ready to schedule your next dental appointment or have questions about our services?
Getting in touch with Smiles N Beyond is simple. Our friendly team is here to help you schedule appointments, answer questions about treatment options, and address any concerns you may have. Whether you prefer to call our office, send an email, or complete our easy online contact form, we’re happy to assist you. Take the first step toward a healthier, more confident smile, contact us today and experience the difference personalized dental care can make.