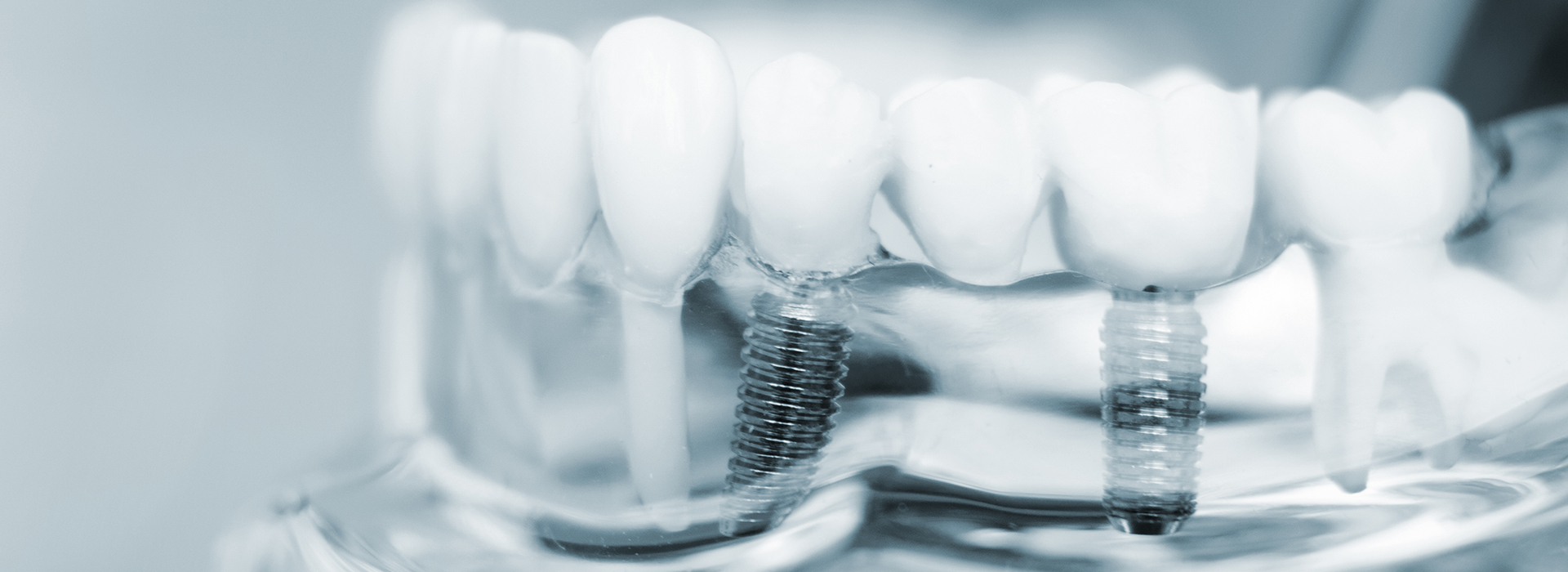
Missing teeth change more than just the look of your smile — they alter how you eat, speak, and care for your oral health. Millions of adults live with gaps that compromise chewing efficiency and can accelerate changes in jawbone shape and facial appearance. Modern implant dentistry offers a reliable path to restoring function and appearance in a way that respects the surrounding teeth and tissues.
Dental implants are engineered to act like tooth roots, providing a stable foundation for crowns, bridges, or full-arch restorations. Because they integrate directly with the jawbone, implants can support chewing forces and help maintain bone volume over time. For many patients, that combination of strength and preservation makes implants the preferred long-term option.
Our practice focuses on careful evaluation and individualized plans so each restoration supports comfortable function and a natural appearance. Smiles N Beyond combines evidence-based techniques with patient-centered communication to make implant treatment clear, predictable, and approachable for people considering tooth replacement.

Unlike removable prostheses, implant-supported restorations behave like permanent teeth. Implant crowns and bridges are anchored to titanium posts that integrate with bone, so the prostheses don’t shift during speech or meals. That stability improves comfort and helps patients reclaim the confidence to bite into foods they may have avoided for years.
Materials used for implant restorations are chosen for durability and aesthetics. Ceramic and porcelain options match neighboring teeth in color and translucency, while modern laboratory techniques let clinicians shape contours and contact points that look and function like natural dentition.
Because implants don’t rely on adjacent teeth for support, they preserve healthy tooth structure that might otherwise need to be altered for a conventional bridge. In many cases, implants protect neighboring teeth and reduce long-term wear on the remaining dentition.
A dental implant starts as a small, biocompatible post placed into the jawbone. Over several months the surrounding bone remodels and bonds to the implant surface — a process called osseointegration. When integration is complete, the implant provides a stable anchor that is capable of supporting a single crown, multiple-unit bridge, or an overdenture.
This direct connection to bone restores mechanical function and helps transmit chewing forces in a healthy way. That stimulation discourages the bone shrinkage that commonly follows tooth loss and can help preserve the facial contours that support a youthful appearance.
Successful outcomes depend on precise planning, careful surgical technique, and appropriate restorative design. Our team emphasizes each of these elements when developing a treatment sequence tailored to a patient’s oral health, anatomy, and personal goals.
Implant restorations offer benefits that go beyond visual improvements. Because implants replace a tooth root as well as the visible crown, they help preserve the health and volume of jawbone. Over time, that preservation translates into better support for facial soft tissues and a reduced tendency for the jaw to shrink in areas of tooth loss.
Where removable dentures can shift or require adhesive, implants provide a fixed or securely retained solution that simplifies daily life. Patients commonly report improved speech clarity and fewer dietary limitations after transitioning to implant-supported restorations.
Unlike natural teeth, implant fixtures are immune to tooth decay. That doesn’t mean implants are maintenance-free — the surrounding gum and bone still require good hygiene and routine professional care to ensure long-term stability.
Implant-supported crowns and bridges allow patients to eat a wide range of foods without worry of slipping or discomfort. They restore normal biting and chewing forces so nutrition choices aren’t unnecessarily restricted, which can have a positive influence on overall health and well-being.
From an oral-health perspective, implants eliminate the need to modify adjacent teeth in many cases. This conservative approach keeps healthy tooth structure intact and reduces the chance of future problems related to overprepared teeth or uneven stress distribution.
When planned and executed with attention to detail, implant therapy can produce predictable results that meet both functional and aesthetic expectations for many years.
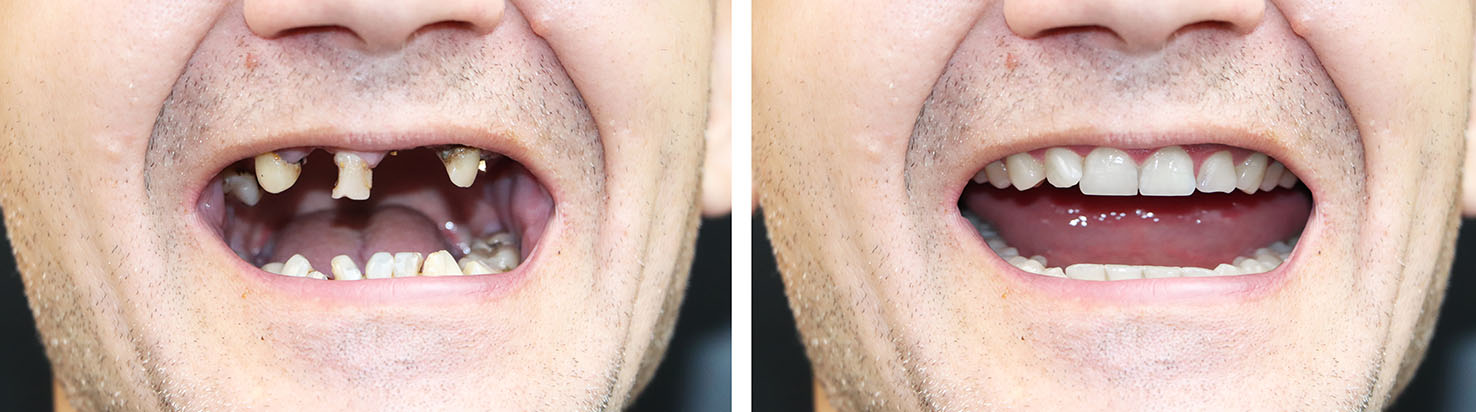
Candidacy for implants is determined by a combination of oral health, bone volume, overall medical history, and lifestyle considerations. Many adults with missing teeth are suitable candidates, but the evaluation includes a review of gum health, existing restorations, and any medical conditions that could affect healing.
Advanced imaging and careful clinical examination are used to assess bone quality and to map vital structures. Where bone is insufficient, adjunctive procedures such as bone grafting or site development can create a stable foundation for implant placement.
We discuss all relevant factors during a consult so you can make an informed decision. Our team takes time to explain risks, benefits, and realistic outcomes based on your individual circumstances.
Implant therapy begins with treatment planning, which may include 3D imaging, study models, and digital mock-ups to visualize the final outcome. The surgical placement of implants is typically performed on an outpatient basis and is considered a routine procedure when executed by an experienced team.
Local anesthesia and, when appropriate, sedation options are used to keep patients comfortable. After implant placement, a healing period allows for osseointegration — the process by which bone bonds to the implant surface. Temporary restorations can often be provided so patients maintain appearance and function during this phase.
Once integration is complete, final restorations are fabricated to precisely fit the implants and surrounding teeth. Follow-up visits focus on checking fit, occlusion, and hygiene access to ensure the long-term health of both the implants and the surrounding tissues.
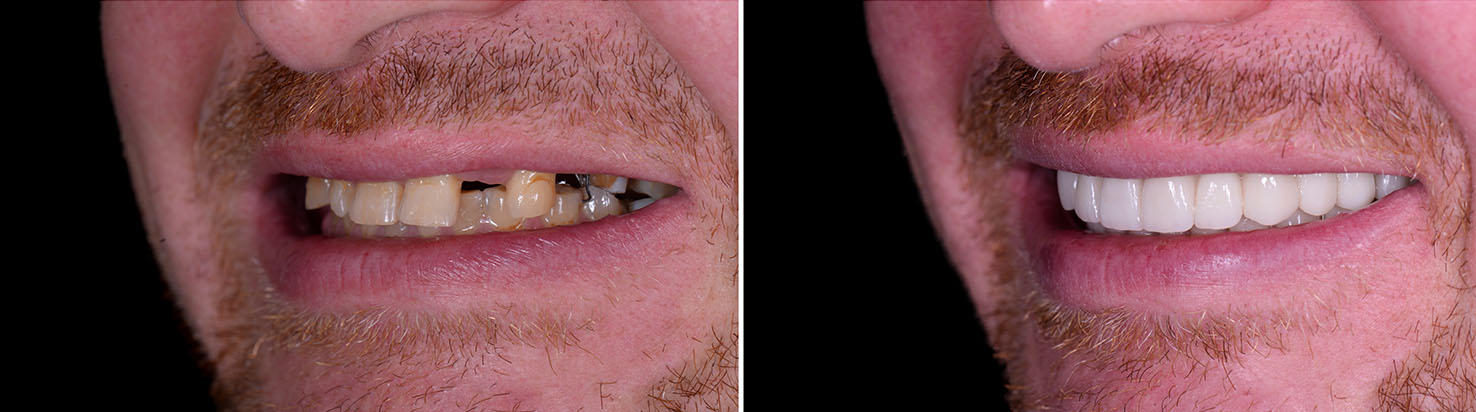
Successful implant placement depends on having adequate bone to support the implant fixture. Tooth loss, periodontal disease, or long-standing gaps can result in bone resorption that makes implant placement more challenging. In those cases, bone grafting or ridge augmentation can rebuild lost volume and create a stable foundation.
Bone grafting materials and techniques vary depending on the site and the amount of augmentation required. The goal is to restore sufficient width and height to ensure the implant can be positioned for optimal support and esthetics. These procedures are commonly performed either before implant placement or at the same time as the implant in carefully selected cases.
When bone grafting is part of the plan, thoughtful staging and communication help patients understand the sequence and expected healing timeline. Careful surgical technique and postoperative maintenance increase the likelihood of long-term success.
Implant longevity relies on regular dental care and consistent home hygiene. Routine checkups allow clinicians to monitor the health of the surrounding gum and bone, check the integrity of restorations, and address any early signs of issues. With proper care, many implant restorations function well for many years.
Our team emphasizes customized maintenance protocols tailored to each patient’s needs. Recommendations may include more frequent professional cleanings, targeted home-care strategies, and periodic radiographic checks to track bone levels and restoration fit.
Dental implants offer a dependable way to replace missing teeth while protecting the health and appearance of your jaw and remaining teeth. If you’re curious whether implants are a good fit for your situation, our team can evaluate your oral health and explain the options that best match your goals and lifestyle. Smiles N Beyond welcomes the opportunity to discuss implant solutions and craft a plan that supports long-term function and a natural-looking smile.
Please contact us to learn more or to schedule a consultation — we’re happy to answer your questions and help you explore the best path forward for your smile.

Dental implants are biocompatible posts that replace missing tooth roots and are placed into the jawbone to provide a stable foundation for restorations. Over time the surrounding bone remodels and bonds to the implant surface in a process called osseointegration, which creates a secure anchor for crowns, bridges, or overdentures. Because implants restore root function they help maintain jawbone volume and support normal chewing and speech.
Implant restorations are custom designed to match neighboring teeth in shape and color, and they can be used for single-tooth replacement, multiunit bridges, or full-arch solutions. The implant system typically includes the fixture, an abutment, and the final prosthesis, each chosen to balance strength, fit, and aesthetics. Careful planning and precise restorative design help ensure the implant functions like a natural tooth over the long term.
Candidacy for implants is based on oral health, bone quantity and quality, and general medical considerations rather than age alone. Healthy gums, adequate jawbone to support the implant, and controlled chronic conditions are favorable factors, while active gum disease or unstable systemic conditions may need to be addressed before placement. Advanced imaging and a clinical exam are used to evaluate bone volume and the location of vital structures to determine suitability.
When bone is insufficient, adjunctive procedures such as bone grafting or ridge augmentation can often create the necessary support for an implant. Lifestyle factors like smoking and certain medications can influence healing and success rates, so these items are discussed during evaluation. A thorough consult lets the dental team tailor a treatment plan that aligns with each patients anatomy and goals.
Treatment begins with diagnostic planning that may include 3D imaging, study models, and digital treatment simulations to map implant position and restorative outcomes. The surgical stage places the implant into the prepared site, after which a healing period allows osseointegration to occur; this phase commonly lasts several months depending on the case and the site. Temporary restorations can often be provided to maintain appearance and function during healing when clinically appropriate.
After integration is confirmed, the restorative phase involves attaching an abutment and fabricating the final crown, bridge, or prosthesis to fit the implant precisely. Follow-up visits check fit, occlusion, and hygiene access to ensure long-term performance. The overall timeline varies with individual needs, adjunctive procedures like grafting, and healing responses.
Implant surgery is performed under local anesthesia and, when appropriate, sedation options are available to enhance patient comfort during the procedure. Most patients experience minimal intraoperative discomfort because the area is numbed, and modern techniques aim to be as atraumatic as possible. After surgery it is common to have mild swelling, soreness, or bruising that can be managed with prescribed or over-the-counter medications and simple postoperative instructions.
Recovery times vary by patient and by the complexity of the procedure, but many people return to normal activities within a few days while following recommended dietary and oral hygiene precautions. The team provides specific aftercare guidance, including how to clean around the surgical site and when to schedule follow-up visits. Prompt reporting of unusual pain, persistent swelling, or signs of infection helps address complications early and supports predictable healing.
Unlike traditional bridges or removable dentures, implants replace the tooth root as well as the crown, which helps preserve jawbone and maintain facial support over time. Implants often allow clinicians to avoid altering adjacent healthy teeth, a common requirement for conventional bridges, and they provide greater stability than many removable prostheses. The fixed or securely retained nature of implant restorations typically improves chewing efficiency and speech clarity compared with unstable dentures.
Removable dentures may still be appropriate for some patients, but implant-supported options can reduce slippage and the need for adhesives while improving confidence with eating and speaking. Implants also transmit functional forces into the bone, which helps reduce resorption in the area of the missing tooth. The choice among implants, bridges, and dentures depends on anatomy, patient goals, and a careful risk-benefit discussion with the dental team.
Implant dentistry offers several restorative options to match different clinical needs, including single implant crowns, implant-supported bridges for adjacent missing teeth, and full-arch fixed prostheses for complete upper or lower restoration. For patients who prefer a removable solution, implant-retained overdentures attach to implants for enhanced retention and stability compared with conventional dentures. The restorative design is selected based on the number of missing teeth, bone availability, and functional and aesthetic goals.
Full-arch solutions can range from a removable overdenture secured by a few implants to a fixed prosthesis supported by multiple implants, sometimes described by approaches such as All-on-4 or similar concepts. Each option has trade-offs in maintenance, hygiene access, and restoration design that are reviewed during the planning phase. The restorative material and contouring are customized to blend with natural dentition and to provide comfortable occlusion.
Long-term implant success depends on consistent home care and regular professional maintenance, much like natural teeth. Daily brushing with a soft-bristled toothbrush, cleaning between implants with floss or interdental brushes, and rinsing as directed help control bacterial accumulation around the implant and surrounding soft tissues. Establishing a routine that preserves gum health and removes plaque is essential for preventing inflammation around the implant.
Professional checkups and cleanings allow the dental team to monitor tissue health, check restoration fit, and perform targeted hygiene where needed. Some patients are recommended more frequent recall visits based on their individual risk profile, oral hygiene habits, or history of periodontal disease. Early detection of changes in tissue or bone levels increases the chance of successful intervention and long-term stability.
Bone grafting or a sinus lift may be recommended when the jawbone lacks sufficient height or width to securely support an implant due to long-standing tooth loss, periodontal disease, or anatomic limitations. Grafting rebuilds the ridge using autogenous, allograft, xenograft, or synthetic materials selected for the clinical situation, while a sinus lift elevates the sinus floor to provide vertical height in the upper jaw. These procedures aim to create a predictable foundation so implants can be placed in an ideal position for function and aesthetics.
Timing for grafting varies; in some cases grafting is performed prior to implant placement to allow healing, while in other situations grafting can be done at the time of implant surgery. The decision is based on the amount of existing bone, the type of restoration planned, and the patients healing capacity. Clear communication about staging and expected healing timelines helps patients understand the overall treatment sequence.
As with any surgical procedure, implant placement carries risks such as infection, nerve or sinus injury, insufficient integration, and peri-implantitis, an inflammatory condition affecting the tissues around an implant. Many risks are minimized through thorough preoperative planning, proper surgical technique, and careful patient selection, including management of systemic factors that influence healing. Early signs of complications are addressed promptly to reduce their impact and to protect surrounding structures.
Long-term complications are often related to inadequate oral hygiene, uncontrolled periodontal disease, or harmful habits like smoking, so prevention focuses on maintenance and patient education. When problems arise, treatment may include nonsurgical therapy, targeted surgical interventions, or restoration adjustments depending on the diagnosis. Regular follow-up and close communication with the dental team increase the likelihood of identifying issues early and achieving favorable outcomes.
During a consultation the team will review your medical and dental history, perform a clinical exam, and obtain diagnostic imaging such as CBCT or radiographs to evaluate bone, tooth relationships, and vital anatomy. The consultation includes a discussion of restorative goals, available implant options, and any preparatory procedures that may be necessary, such as grafting or periodontal care. This appointment is an opportunity to ask questions about the sequence of care, comfort measures, and what to expect at each stage of treatment.
At Smiles N Beyond in Wallington, NJ the focus is on creating a clear, personalized plan that aligns clinical needs with patient preferences and long-term function. The team will explain follow-up steps, estimated timelines for healing and restoration, and recommended maintenance protocols to support lasting results. If you decide to move forward, the practice coordinates imaging and scheduling so treatment can begin in a well-organized manner.

Ready to schedule your next dental appointment or have questions about our services?
Getting in touch with Smiles N Beyond is simple. Our friendly team is here to help you schedule appointments, answer questions about treatment options, and address any concerns you may have. Whether you prefer to call our office, send an email, or complete our easy online contact form, we’re happy to assist you. Take the first step toward a healthier, more confident smile, contact us today and experience the difference personalized dental care can make.