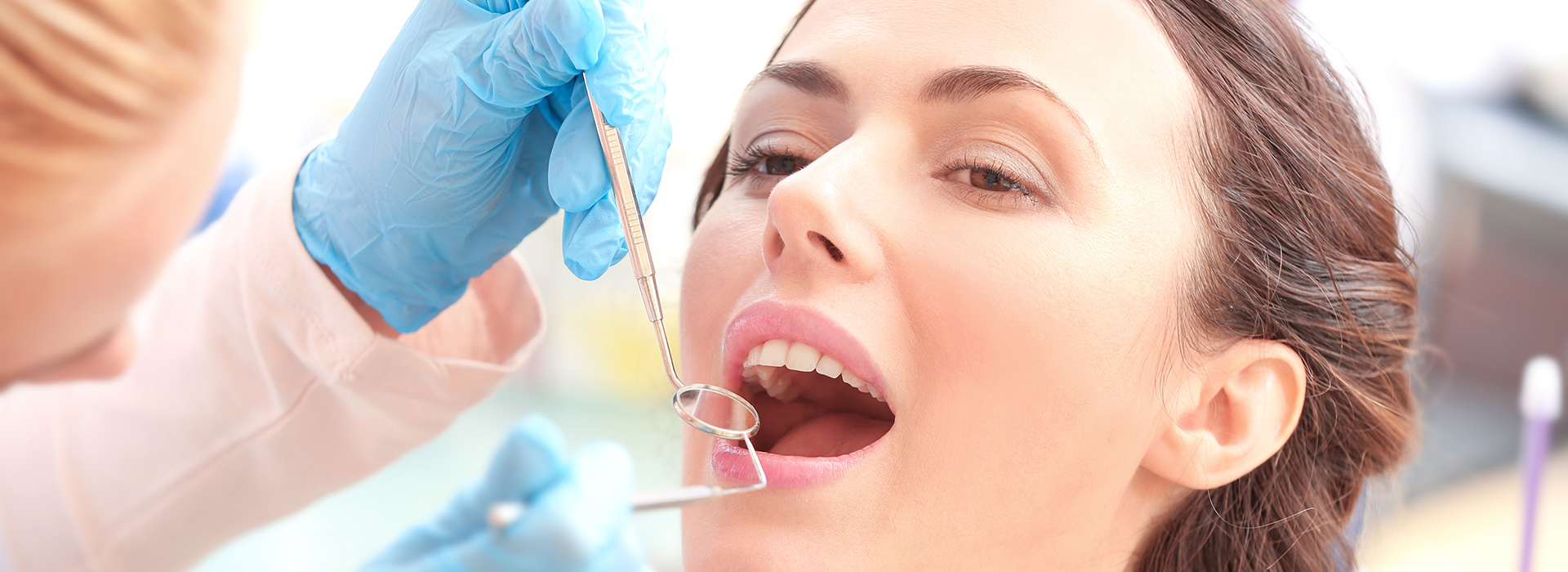
Gum disease is the most common reason adults lose teeth, and it often advances quietly. According to data from the Centers for Disease Control and Prevention, roughly half of adults over age 30 show signs of periodontal disease. The condition ranges from reversible inflammation to destructive forms that damage bone and soft tissues around the teeth. At Smiles N Beyond in Wallington, NJ, our team provides attentive periodontal care aimed at preserving natural teeth and supporting long-term oral health.
Periodontal disease begins when dental plaque — a sticky film of bacteria — accumulates at and below the gumline. The tissues that surround and support teeth (the periodontium) react to this bacterial presence with inflammation. Over time, ongoing inflammation can break down the connective tissues and bone that anchor teeth, creating spaces called periodontal pockets where bacteria multiply.
Because early stages often cause minimal discomfort, many people are unaware that a problem is developing. That is why routine exams and cleanings are so important: they allow a dental professional to detect changes in pocket depth, gum attachment, and bone levels long before symptoms become severe.
Recognizing the early warning signs can make a major difference. If you notice any persistent redness, bleeding, swelling, or a change in how your teeth fit together, bring this to your dental provider’s attention so the condition can be assessed and addressed promptly.
Red, swollen, or tender gums
Bleeding during brushing or flossing
Gums that appear to pull away from the teeth or expose root surfaces
Persistent bad breath or an unpleasant taste
Tooth sensitivity, looseness, or changes in bite

Gum health is more than an aesthetic concern — it contributes to overall health. Research links chronic oral inflammation to systemic conditions such as diabetes management, cardiovascular health, and certain respiratory issues. While the relationships are complex and still being studied, reducing oral inflammation is a practical step patients can take to support broader health goals.
Preventing and controlling periodontal disease helps preserve the structures that keep teeth stable and functional. Beyond saving teeth, effective periodontal care simplifies daily hygiene, reduces infection risk, and improves comfort when eating and speaking.
At Smiles N Beyond we emphasize prevention and early intervention. Routine periodontal screenings, thoughtful hygiene instruction, and consistent professional care work together to reduce risk and maintain a healthier mouth over time.
Gingivitis is the initial, reversible stage of periodontal disease. It shows up as gum inflammation without the loss of bone or connective tissue that secures teeth. Typical signs include bleeding during brushing, mild swelling, and a tendency for gums to look darker or feel tender.
The good news is that gingivitis responds well to improved oral hygiene and professional cleanings. When plaque and calculus (tartar) are removed and daily home care is optimized, the inflammatory response usually subsides and tissue health is restored.
Early treatment often consists of a focused dental cleaning to remove deposits below the gumline, paired with personalized instructions on brushing, interdental cleaning, and other home care measures. With diligent follow-up, most cases of gingivitis do not progress to more destructive disease.

When gingivitis is left untreated, it can develop into periodontitis — a stage where the inflammatory process damages the connective tissues and bone that support teeth. As attachment is lost, pockets deepen and teeth may shift, feel loose, or become more sensitive. In many cases, bone loss can be seen on radiographs by a dental professional.
Treatment at this stage focuses on stopping the disease and restoring as much support as possible. Approaches vary by severity but can include deeper cleaning below the gumline, antimicrobial therapies, and, when necessary, surgical procedures to reduce pocket depth and regenerate lost tissues.
Timely intervention improves the chance of stabilizing the condition and preserving remaining support. Ongoing maintenance is essential after active therapy to monitor healing and prevent recurrence.
Contemporary periodontal care offers a range of therapies that go beyond cleaning to actively restore damaged tissues. Bone grafts, guided tissue regeneration, and soft tissue grafts are among the techniques used to rebuild lost volume and reestablish healthy attachments when indicated. These procedures can improve function, reduce sensitivity from exposed roots, and enhance the smile’s appearance.
Dental lasers are another tool that may be used selectively to remove diseased tissue, reduce pocket depths, and treat areas around dental implants. When applied appropriately, laser therapy can complement conventional approaches and may offer benefits like reduced bleeding and more precise tissue management.
Every treatment plan is tailored to the individual. Your provider will consider the extent of tissue loss, overall health, and your goals to recommend restorative and supportive options that align with your needs.
Non-surgical approaches are the first line of treatment for most patients with mild to moderate periodontal disease. These methods are practical and focused on removing the bacterial deposits that provoke inflammation. Deep cleanings, often called scaling and root planing, clear plaque and hardened calculus from below the gumline and smooth root surfaces to discourage reattachment of bacteria.
Adjunctive measures can include locally applied antimicrobials placed in pockets to reduce bacterial load or systemic medications in select situations. Equally important is improving daily plaque control at home — consistent brushing, interdental cleaning, and professional maintenance visits are required to sustain the benefits of non-surgical therapy.
When patients respond well to conservative care, invasive procedures may be unnecessary. However, close monitoring is essential to ensure healing and to identify any sites that need further intervention.
Surgery becomes a consideration when pocket depths are too great for thorough cleaning with non-surgical methods or when regenerative procedures can meaningfully improve outcomes. Periodontal surgery allows the clinician to access root surfaces and bone for thorough debridement, reshape damaged tissues, and, when appropriate, place grafting materials to encourage new bone and connective tissue growth.
One commonly used technique, flap surgery, temporarily repositions gum tissue to provide direct access for cleaning and repairs. After the necessary work is completed, the tissue is repositioned and sutured to optimize healing and reduce pocket depth.
The goals of surgical therapy include removing persistent bacterial reservoirs, halting further bone loss, and creating an environment that patients can maintain effectively at home. With proper surgical care and ongoing maintenance, many patients achieve long-term stability and improved comfort.
Eliminate bacterial deposits beneath the gums and on root surfaces
Arrest bone loss and reshape supporting structures as needed
Reduce pocket depth to enable effective daily cleaning and maintenance
When deciding on surgical options, your dental team will discuss expected benefits, recovery considerations, and follow-up care so you can make an informed choice about the best path forward.
Periodontal care is a partnership between you and your dental team. Early detection, consistent home care, and individualized treatment plans give the best chance for a healthy, long-lasting smile. If you would like to learn more about periodontal treatment options or schedule an evaluation, please contact us for more information.

Periodontal disease is an infection of the tissues that surround and support the teeth, beginning with inflammation of the gums and potentially advancing to the loss of bone and connective tissue. Early stages, known as gingivitis, are characterized by redness, swelling and bleeding while more advanced periodontitis involves pocket formation, attachment loss and possible tooth mobility. Progression occurs when bacterial biofilm persists below the gumline and the body’s inflammatory response gradually destroys supporting structures.
Because early periodontal disease often causes only mild symptoms, routine dental examinations and periodontal screening are critical for detecting changes in pocket depth, gum attachment and bone levels. Timely identification allows providers to recommend conservative treatments that can halt or reverse damage in many cases. Ongoing monitoring after treatment helps detect recurrence and guides maintenance care.
The primary cause of periodontal disease is the accumulation of bacterial plaque and calculus at and below the gumline, which provokes an inflammatory response in the periodontium. Several risk factors increase susceptibility, including tobacco use, poorly controlled diabetes, certain medications, genetic predisposition, inadequate oral hygiene and advancing age. These factors can influence the severity of tissue breakdown and the response to treatment.
Systemic health conditions that affect the immune response or circulation can make periodontal disease more difficult to control, and habits such as smoking reduce healing potential after therapy. Identifying and addressing modifiable risks is an important part of a comprehensive periodontal plan. Your dental team will review your medical history and lifestyle factors to tailor prevention and treatment strategies.
Diagnosis typically involves a clinical periodontal exam and radiographic imaging to evaluate pocket depths, bleeding on probing, gum attachment levels and bone support around the teeth. The dentist or hygienist will use a periodontal probe to measure pocket depths and document any sites with increased pocketing or attachment loss, and X-rays help reveal bone changes not visible during a visual exam. A complete assessment also includes reviewing your medical history and any symptoms such as soreness, sensitivity or changes in bite.
At Smiles N Beyond in Wallington, NJ, these screening steps are part of routine exams so that early signs can be detected and addressed before they become more destructive. The diagnostic information guides whether non-surgical therapy, adjunctive measures or referral for periodontal specialty care is the most appropriate next step. Clear documentation of baseline measurements also enables effective tracking of treatment response over time.
Non-surgical therapy is the first-line approach for most cases of mild to moderate periodontal disease and centers on removing bacterial deposits from root surfaces below the gumline. Scaling and root planing (deep cleaning) removes plaque and tartar and smooths the roots to reduce bacterial reattachment, while adjunctive measures such as locally delivered antimicrobials may be used in specific pockets to lower bacterial load. Emphasis is also placed on patient-centered home care instruction so daily plaque control supports professional treatment outcomes.
In select situations, systemic antibiotics or host-modulation strategies can be considered as adjuncts to mechanical therapy, but these are used judiciously based on the individual’s condition and medical history. Response to non-surgical care is monitored closely, and maintenance visits are scheduled to reinforce hygiene and ensure the disease is controlled. When conservative therapy achieves stable results, many patients can avoid more invasive procedures.
Surgery is considered when pocket depths or anatomical factors prevent thorough cleaning with non-surgical methods, or when regenerative procedures can meaningfully restore lost tissue. Common surgical approaches include flap surgery to gain access for deep debridement, bone grafting and guided tissue regeneration to encourage new bone and connective tissue growth, and soft tissue grafts to address gum recession and root sensitivity. The chosen procedure depends on the extent of tissue loss, the patient’s health status and the clinical goals for function and aesthetics.
Surgical care aims to eliminate persistent bacterial reservoirs, reduce pocket depth to a maintainable level and reconstruct supporting structures when possible. Your dental team will discuss expected benefits, potential risks, and postoperative care so you can make an informed decision. With proper surgical technique and a structured maintenance plan, many patients achieve long-term stability and improved comfort.
Dental lasers can be used selectively as an adjunct to conventional periodontal therapy to remove diseased soft tissue, reduce bacterial counts in pockets and enhance tissue management during certain procedures. When applied appropriately, lasers may offer advantages such as precise tissue targeting and reduced bleeding, but they are not a universal replacement for mechanical debridement. Clinical evidence supports laser use in specific situations, and clinicians evaluate each case to determine whether laser therapy is a suitable complement.
Lasers may also play a role in treating peri-implant soft tissue inflammation under particular protocols, but long-term outcomes depend on comprehensive care that includes mechanical cleaning and patient home care. Your provider will explain how laser options fit into your individualized treatment plan and whether adjunctive laser therapy is likely to improve healing or comfort in your case. Selection of technology is guided by clinical findings and the goal of predictable results.
Effective periodontal therapy stops or slows tissue destruction, preserves remaining bone and connective tissue, and reduces the likelihood of tooth loss associated with advanced disease. By lowering inflammation and pocket depths, treatment improves the ability to clean teeth at home, reduces sensitivity from exposed roots and enhances comfort when chewing and speaking. Restoring a stable foundation also supports future restorative or prosthetic work when needed.
Beyond local benefits, controlling periodontal infection can simplify daily hygiene and decrease the frequency of acute periodontal episodes that require urgent care. Long-term maintenance and regular reassessment are essential to sustain the gains achieved during active therapy. Collaborative care between the patient and dental team is central to maintaining oral function and overall periodontal stability.
After non-surgical therapy patients commonly experience mild soreness, gum tenderness and temporary sensitivity that can be managed with over-the-counter pain relievers as advised by the clinician and by following home care instructions. Healing from scaling and root planing generally progresses over several weeks, during which soft tissues reattach and inflammation subsides; follow-up visits assess healing and determine whether additional therapy is needed. After surgical procedures, short-term swelling, discomfort and minor bleeding are typical and detailed postoperative guidelines help promote uneventful recovery.
Your dental team will provide specific instructions for oral hygiene, diet and activity after treatment and will schedule follow-up appointments to monitor healing and remove sutures if applicable. Proper home care and adherence to recall visits are important to protect the treatment site and to achieve predictable long-term results. If unexpected symptoms such as severe pain, persistent bleeding or signs of infection arise, contact the office promptly for evaluation.
Daily plaque control is the foundation of preventing periodontal recurrence and includes brushing twice a day with a soft-bristled brush, cleaning between teeth with floss or interdental brushes, and using adjunctive tools recommended by your clinician. Technique matters: removing biofilm thoroughly without damaging soft tissues helps maintain health, and regular evaluation ensures your routine remains effective. Smoking cessation and good control of systemic conditions such as diabetes also contribute significantly to periodontal stability.
Consistent attendance at professional maintenance appointments allows your dental team to remove residual deposits, reassess periodontal measurements and reinforce home care strategies. If specific sites show renewed inflammation, targeted interventions can be implemented early to prevent progression. A partnership between patient and provider is the most reliable way to sustain gum health over time.
Frequency of maintenance visits is individualized but patients treated for periodontitis commonly return every three months for supportive periodontal therapy while disease activity is being controlled. These maintenance visits typically include professional cleaning below the gumline, periodontal charting to monitor pocket depths and bleeding, and review of home care practices to ensure consistent plaque control. The interval may be adjusted based on clinical response, risk factors and stability of the condition.
Long-term success depends on an ongoing program of professional care combined with effective daily hygiene, and your dental team will recommend a recall schedule tailored to your needs. Adhering to the recommended maintenance timeline helps catch recurrence early and preserves the improvements achieved through active therapy. Smiles N Beyond can work with patients to establish a maintenance plan that aligns with their oral health status and goals.

Ready to schedule your next dental appointment or have questions about our services?
Getting in touch with Smiles N Beyond is simple. Our friendly team is here to help you schedule appointments, answer questions about treatment options, and address any concerns you may have. Whether you prefer to call our office, send an email, or complete our easy online contact form, we’re happy to assist you. Take the first step toward a healthier, more confident smile, contact us today and experience the difference personalized dental care can make.